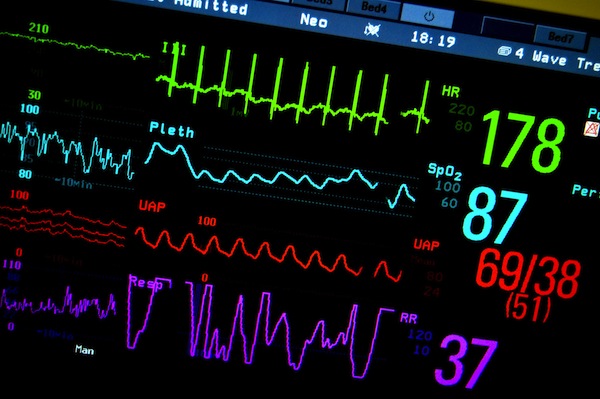
 Once you create a situation at law where killing of another person is allowed in certain circumstances, not only will the circumstances in which such killing is endorsed or allowed change over time, but the boundaries, however originally drawn, will be entirely ineffective in providing moral, legal and ethical guidance and restraint.
Once you create a situation at law where killing of another person is allowed in certain circumstances, not only will the circumstances in which such killing is endorsed or allowed change over time, but the boundaries, however originally drawn, will be entirely ineffective in providing moral, legal and ethical guidance and restraint.
Already a subscriber? Log in
Get 10 issues
for $10
Subscribe to The Spectator Australia today for the next 10 magazine issues, plus full online access, for just $10.
- Delivery of the weekly magazine
- Unlimited access to spectator.com.au and app
- Spectator podcasts and newsletters
- Full access to spectator.co.uk
Or





















Comments
Don't miss out
Join the conversation with other Spectator Australia readers. Subscribe to leave a comment.
SUBSCRIBEAlready a subscriber? Log in